Clipped from: https://economictimes.indiatimes.com/industry/healthcare/biotech/healthcare/the-covid-19-crisis-has-underlined-the-need-for-more-budgetary-allocation-for-healthcare/articleshow/80074434.cmsSynopsis
Covid-19 showed the Indian healthcare system bursting at its seams at the height of the pandemic; patients turned away, doctors and nurses exhausted in their PPE kits.


COVID-19 CASES
WorldIndiaPandemics have a way of exposing glaring fault lines. When it comes to the healthcare system, it bares every rot in the system, every loose nail, every creaky rafter, every patient in need of aid and every healthcare worker who is overworked. Covid-19 showed the Indian healthcare system bursting at its seams at the height of the pandemic; patients turned away, doctors and nurses exhausted in their PPE kits.
The virus took a heavy toll: over 1 crore people have been infected and about 1.5 lakh have died. The Covid-19 crisis has underlined like never before the need for more budgetary allocation for healthcare. When the pandemic began to spread like wildfire, the Centre announced a stimulus package of Rs 20 lakh crore in May, of which Rs 15,000 crore was allotted towards the country’s “Covid-19 Emergency Response and Health System Preparedness”. Only about half of it — Rs 7,774 crore — was meant for 2020-21, the rest was to be disbursed over the following four years. But this was last-minute firefighting. To bring about qualitative improvement in public healthcare, India needs systemic, multifold allocation and investments.
“India’s public health allocations for the past one decade has been in the range of 0.9-1.3% of GDP while the overall healthcare spending has been 3.8-5%,” says Professor K Srinath Reddy, president, Public Health Foundation of India. Also, health being a state subject, funds often remain unutilised by state governments, points out Bijit Roy, associate director, Population Foundation of India. At 1.6% of GDP for FY2021, public spend on healthcare in India is abysmally low. Even Bhutan and Ethiopia spend more on health. “As things stand, primary health centres can’t handle secondary and tertiary healthcare needs. Government hospitals that offer quality tertiary care are only a handful: AIIMS, Safdarjung Hospital and Ram Manohar Lohia Hospital in Delhi, PGIMER Chandigarh, JIPMER Puducherry, etc.
“Public health system is one area where both states & Centre should invest more. But we need to devise focused policies rather than just increase budget allocation. Doubling the health budget will only double the inefficiency. Unless we improve the quality, doubling expenditure won’t help much”
— ARVIND VIRMANI, former chief economic adviser, GoI
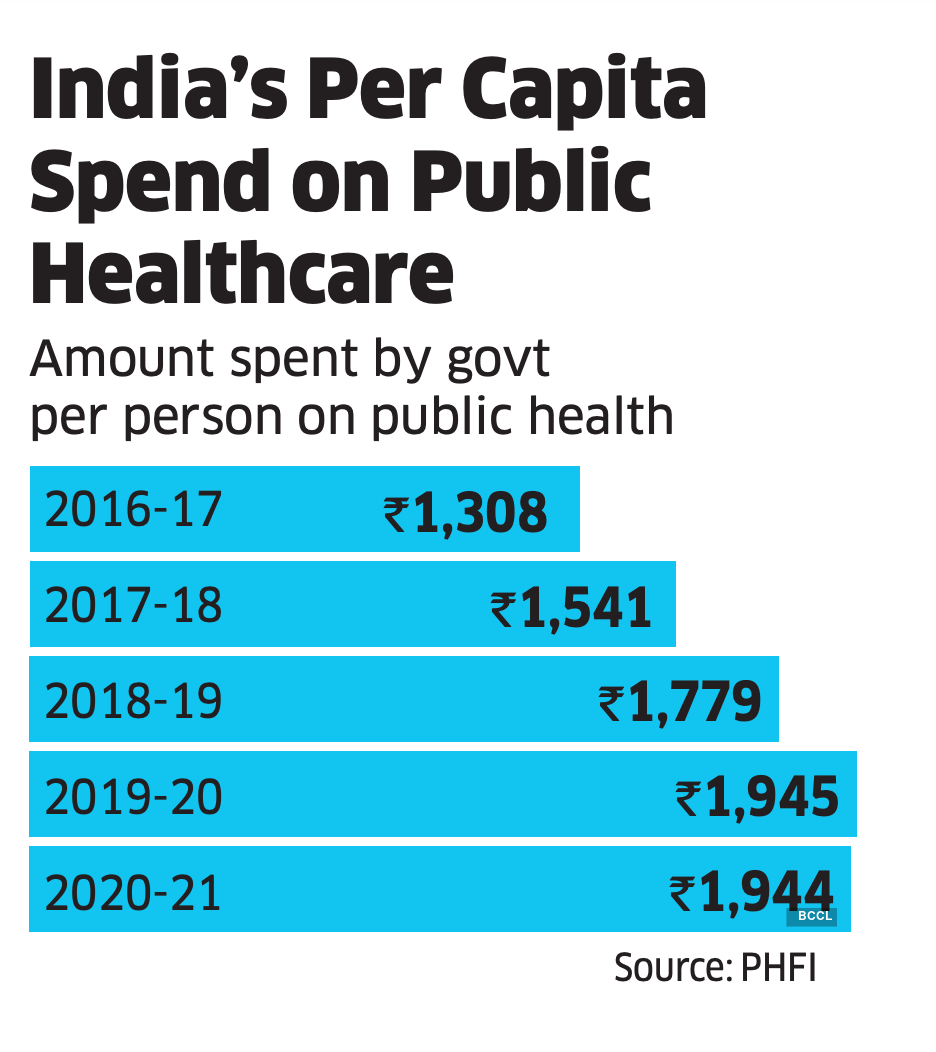
India needs much more investment to ramp up public healthcare,” says former Union health secretary Keshav Desiraju. Even as India’s expenditure has inched up from 1.3% of GDP in 2015, it is still a pale shadow of countries like the US, which sets aside 14% of GDP for health. India spends the least among BRICS countries: Brazil spends 9.2%, South Africa 8.1%, Russia 5.3% and China 5%. India’s per capita government expenditure, at Rs 1,945 in FY21, is also the least among BRICS nations. When government-run primary health centres (PHCs) can’t cater to people’s needs and government hospitals remain burdened by high demand, people have to depend on private healthcare although it is a financial burden for many. Out-of-pocket expenditure (OOPE) is very high in India.
“India needs to spend more on public health at both the Central and state levels. Primary and secondary healthcare systems of states need to be beefedup at the earliest”
— K SRINATH REDDY, President, Public Health Foundation of India
OOPE is borne directly by an individual without any aid from the insurer or the government. More than two-thirds of the population have to bear the cost of health services on their own. “WHO’s health financing profile shows that India’s overall out-of-pocket expense has for several years hovered around 60% while the world average is just 18.2%. India’s spending has been poor on healthcare. Even low-income countries like Sri Lanka (42.1%) are better in this regard,” says Reddy. In comparison, OOPE in China is 32%, Brazil 25.5% and US only 11%. Even as OOPE in India has been decreasing since 2004, it is worryingly high at a time when a large section of the society is vulnerable due to the pandemic.
Health Matters
– 7,13,986 Total govt hospital beds in India
– 0.6 Hospital beds per 1,000 people
-1.5 lakh Primary health centres
– 29,414 Health and wellness centres
– 11.57 lakh Allopathic doctors with state medical councils
– 1:1,457 Ratio of doctor to people (as against WHO norm of 1:1,000)
– 2.5% of GDP Targeted spending on health by 2025
– 70% Healthcare expenses met by out-of-pocket expenses
– 35% Coverage of Ayushman Bharat
(Source: MoHFW)
The Covid outbreak has brought the focus back on healthcare. In pre-budget meetings with Finance Minister Nirmala Sitharaman in the third week of December, a detailed pitch was made industry representatives to give a big boost to healthcare investment and expenditure. “The allocation is bound to be more.
A detailed pitch for higher allocation due to the Covid crisis was shared with the FM in the stakeholders’ consultation meeting. Public healthcare, infrastructure, spending and vaccination will be in focus in the upcoming budget,” says a source, on the condition of anonymity. The 15th Finance Commission has advocated PPP in the health sector, said its chairman NK Singh recently, adding, “The commission has been working toward a financing model to raise public health spending to about 2.5% of GDP over the next five years.”
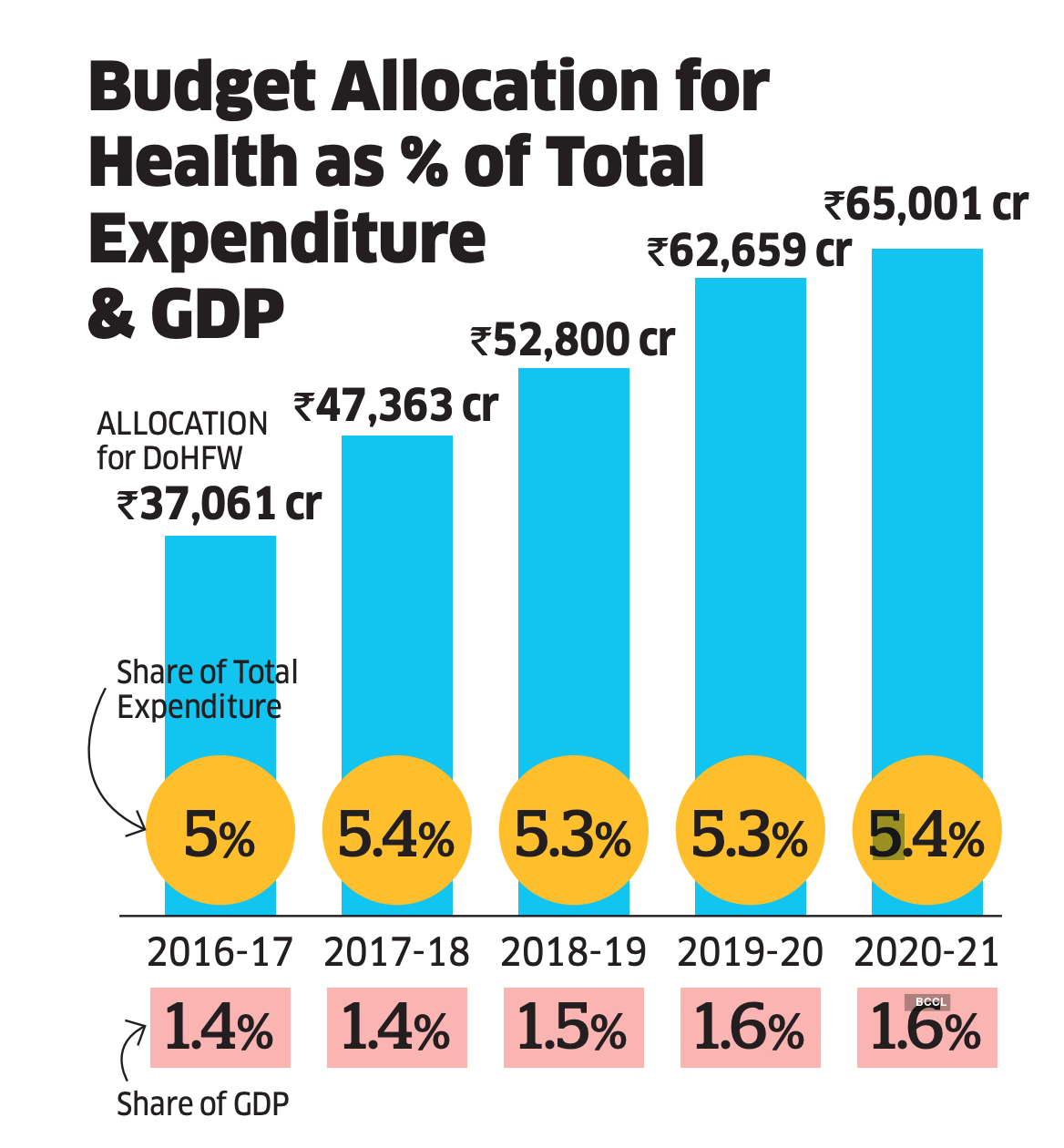
An overstretched public healthcare system needs not just investments to boost infrastructure and human resources but also utilisation of funds. “Limited funding coupled with low public spending by governments for years have hit the quality and reach of required healthcare services,” says Roy of Population Foundation of India. “Many states do not spend more than 50% of allocated funds. This has resulted in widespread inequality in the distribution of health infrastructure and health personnel. We need to look at the geographical spread of healthcare reach and create incentives for doctors in public healthcare. Also, there is a need for massive regulation in private healthcare.”
Rural-Urban Divide
Medical training infrastructure needs a big leg-up too. Even as the number of medical colleges in India went up to 560 in 2020 from 412 in 2015-16, lack of adequate seats in government colleges forces students to opt for private medical colleges that charge an exorbitant fee. “Those who enrol for private colleges are unlikely to return to government-run PHCs. Unless the government regulates this, the situation in rural healthcare won’t improve,” says Desiraju. The only way to solve the problem of poor quality of rural government health services is through e-health/e-medicine, says Arvind Virmani, former chief economic adviser.
“We are expecting a higher allocation for healthcare in this budget. The focus is likely to be on building a strong medical infrastructure and training moredoctors, nurses and paramedical staff”
— Dr NARESH TREHAN, CMD, Medanta
“The government can create a platform which provides access to quality advice from citybased doctors, with local health practitioners intermediating in their two-way communication with rural patients,” he says. In November last year, national telemedicine services completed 8 lakh teleconsultations since its launch. This needs to be ramped up.
Healthcare availability is skewed in favour of urban areas even though three-fourths of the population live in rural areas. According to a study by the Academy of Family Physicians of India, the proportion of households that reported spending out-of-pocket on health rose from 64% in 2005 to 81% in 2012 in rural areas and from 65% in 2005 to 78% in 2012 in urban areas. Also, OOP expense as a share of total household expenditure was higher in rural areas — at 6.34% in 2005 and 7.73% in 2012 — than urban areas — 5.05% in 2005 and 5.74% in 2012.
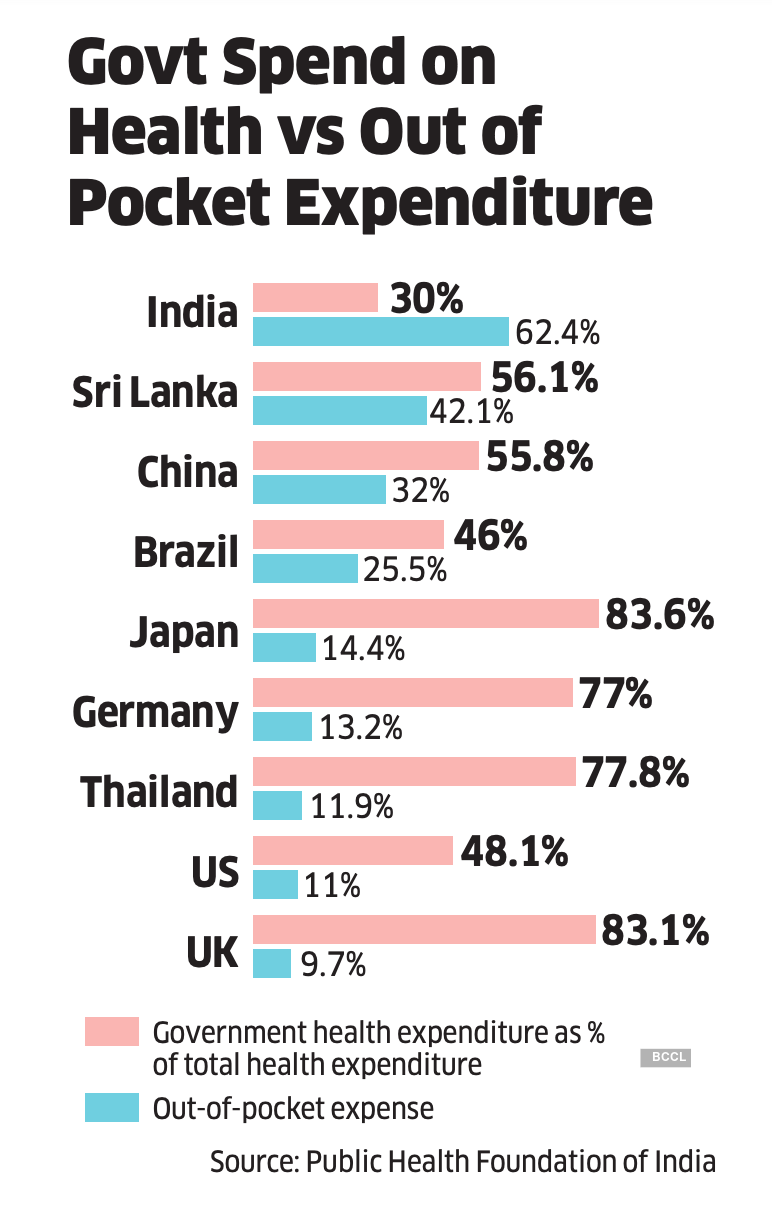
Ayushman Bharat or PMJAY aims to reduce OOPE through cashless services. Launched in 2018, the Centre’s flagship scheme provides cashless cover — of up to Rs 5 lakh per family per year for secondary and tertiary care hospitalisation — to over 10 crore families. Currently, its actual coverage is only around 20%. “PMJAY currently covers 12 crore households (about 50 crore people). But this is nominal coverage. Actual coverage is much low,” says Sakthivel Selvaraj, director, health economics, financing and policy, PHFI. “Although the entire 12 crore-plus households may have an Ayushman Bharat card, many may not be aware of its usage. Households reporting insurance coverage was roughly 20%.”
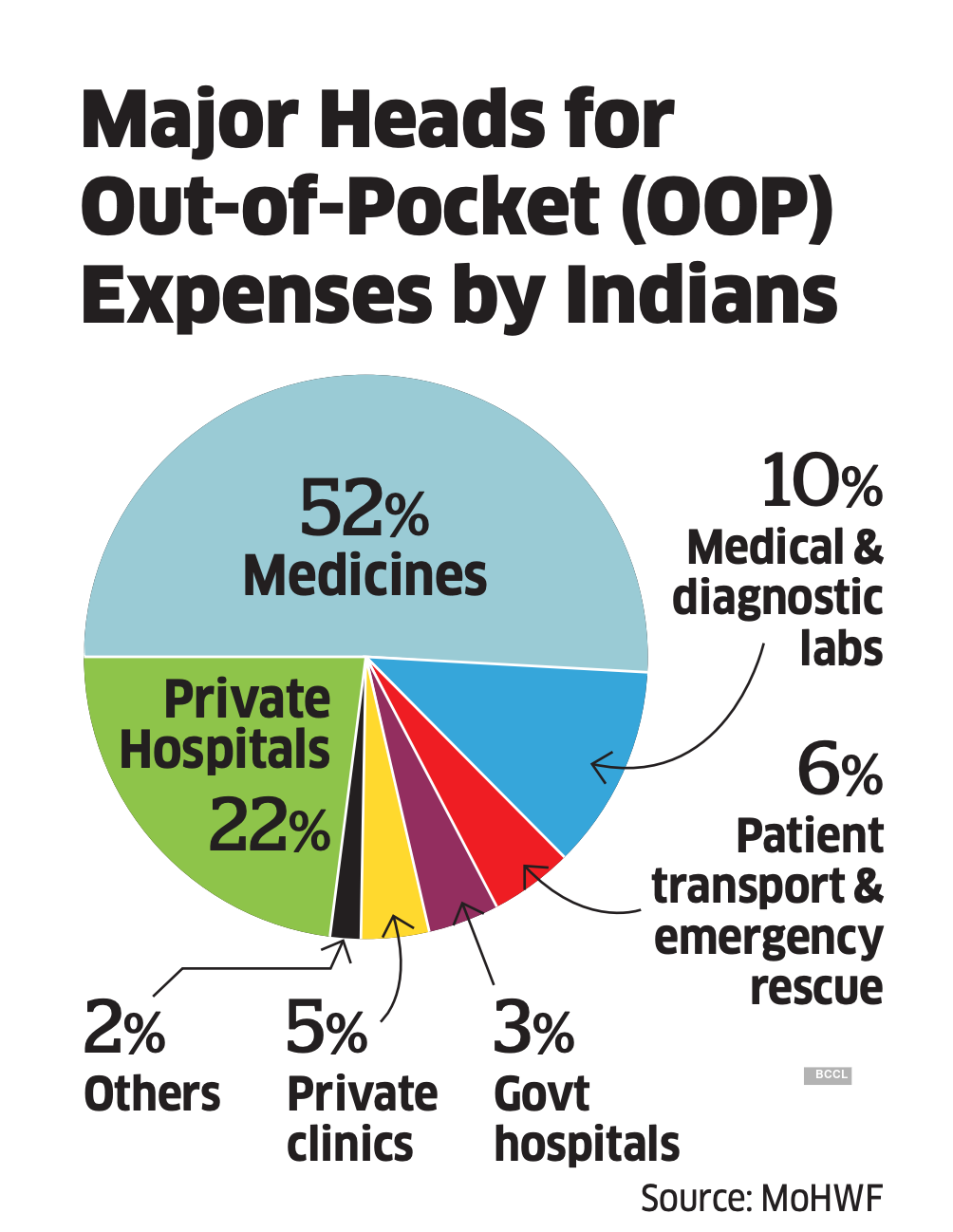
In fact, only 48 crore individuals or 37.2% of India’s population were covered under any health insurance, government or private, in 2018. “We must increase insurance coverage to cut down on individual’s out-of-pocket expenses,” says Virmani. Health insurance is gaining momentum in India, with gross direct premium income underwritten by health insurance growing by 17.16% y-o-y to Rs 51,637.84 crore in FY20. Still, more than 60% of the population has no insurance cover. “The 15th Finance Commission is revising its recommendations, asking for a greater allocation for health both at the central and state levels. If that report delivers what it promises, there would be a shift in the direction of healthcare financing towards universal health coverage,” says Reddy of PHFI.
“We need to spend much more than we do on public health. Programmes such as Integrated Disease Surveillance Programme need a big boost”
— KESHAV DESIRAJU, former Union health secretary
Governments the world over were forced to spend more on healthcare in the past year. This kind of allocation might have otherwise taken decades. “The government is on it. We are expecting a higher allocation for healthcare in this budget. The focus is likely to be on building a strong medical infrastructure and training more doctors, nurses and paramedical staff — that’s what the understanding is,” says Dr Naresh Trehan, CMD, Medanta Hospital. “This virus has caused havoc in the whole county. We have to be ready for other pandemics in the future. The government is aware of future challenges and the need for more allocation. It has already set an agenda of reaching 2.5% healthcare spending of GDP.” As things stand, healthcare in India is marked by poor public health infrastructure, high costs and low insurance coverage.
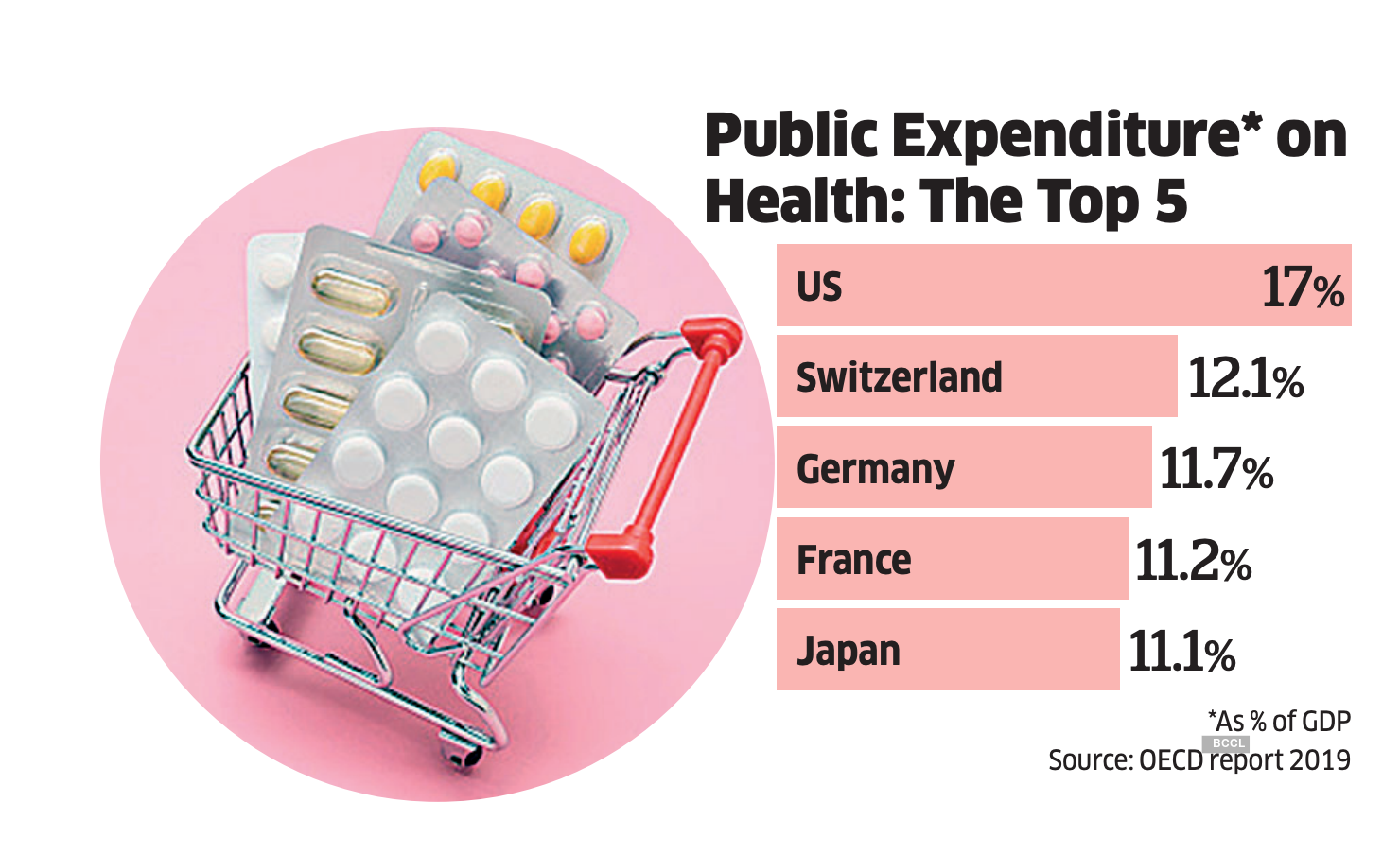
The poor quality of services at public health centres and low insurance coverage lead to high OOPE and increasing use of private hospitals. Private sector’s share in healthcare in India is 78% in urban areas and 71% in rural areas. Experts feel the segment is highly unregulated. “Clinical Establishments (Registration & Regulation) Act 2010 makes it mandatory for private players to furnish every detail. Someone has to enforce the law. Private sector hospitals that come up on highly subsidised land allocated by government must be regulated.
There is hardly any data on EWS quota. This act is one tool available with the government,” says Desiraju. Growth of private sector widens the gap between those who can and cannot afford healthcare. “India would need a combination of innovation and regulatory reforms to address these challenges,” says Virmani. As per the Global Health Expenditure database 2016 of WHO, India ranks 170 of 188 countries in domestic general government health expenditure as a percentage of GDP (it indicates, says World Bank, the priority of the government to spend on health from own domestic public resources). The government aims to raise the public health expenditure to 2.5% of GDP by 2025 in a timebound manner.
WHAT INDIA NEEDS
– Upgrade of PHCs : More budgetary allocation for public healthcare
– More expenditure by states: Increased coverage under Ayushman Bharat
– Investment in medical research
– Regulation of private healthcare
– More doctors / seats in medical colleges
But experts feel India needs a targeted approach to correct inequalities in the distribution of health infrastructure and health personnel rather than merely increasing allocation. “The public health system is one area where both states and Centre should invest more. But we need to devise focused policies rather than just increase budget allocation. Doubling the health budget will only double the inefficiency. Unless we improve the quality, doubling expenditure won’t help much,” says Virmani.